WHAT ARE ZYGOMATIC IMPLANTS?
Let’s start by locating ourselves:
Zygomatic implants have this name because they are implants placed in the zygomatic bone. For those of you who are older, I’m sure you remember the old Anatomical Standard (before 1998), in which the Zygomatic bone was called the Malar bone. It’s not incorrect to call it the Malar bone, from a lay and social point of view, but in medical and surgical terms the bone is now called the Zygomatic bone.
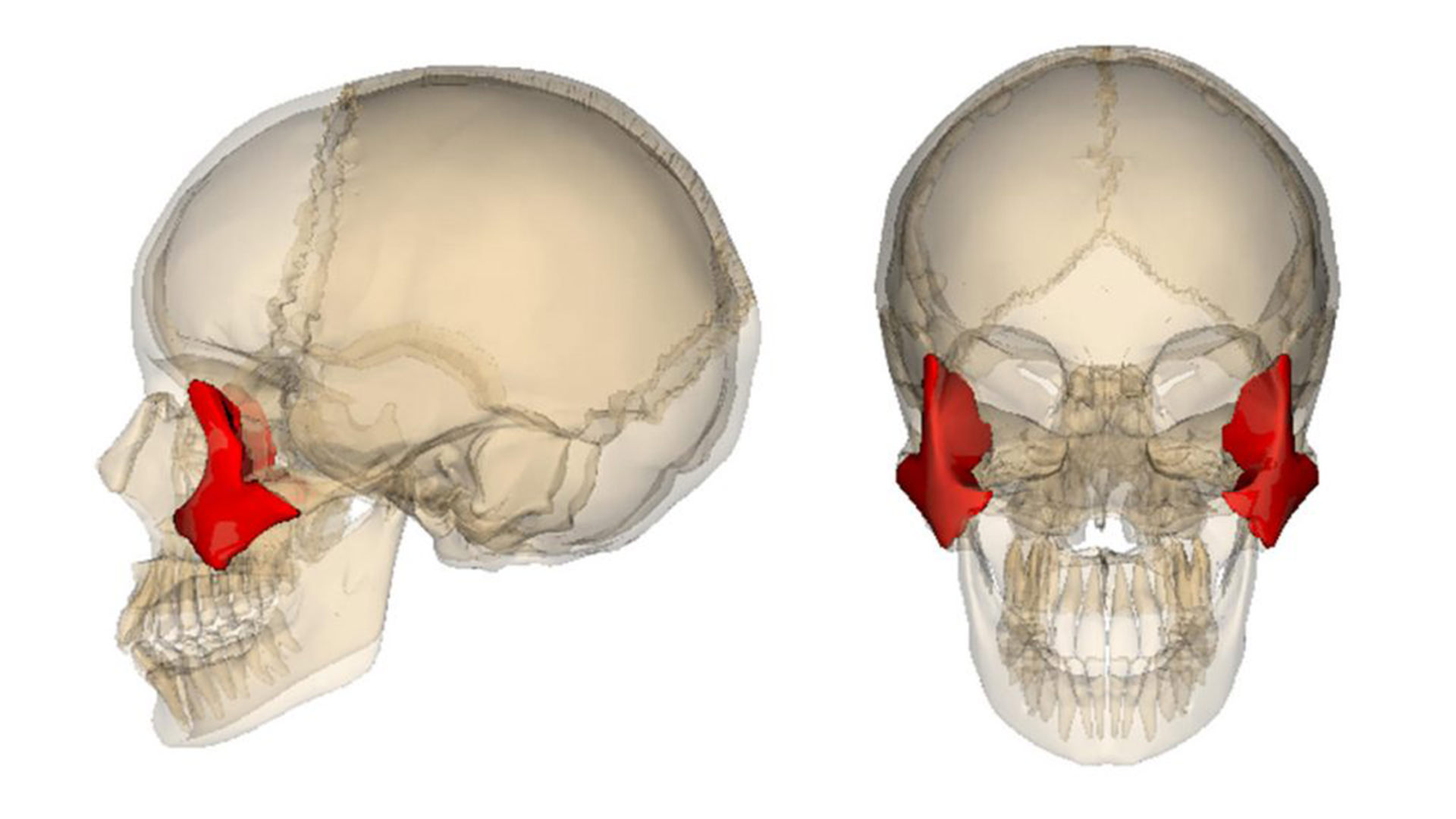
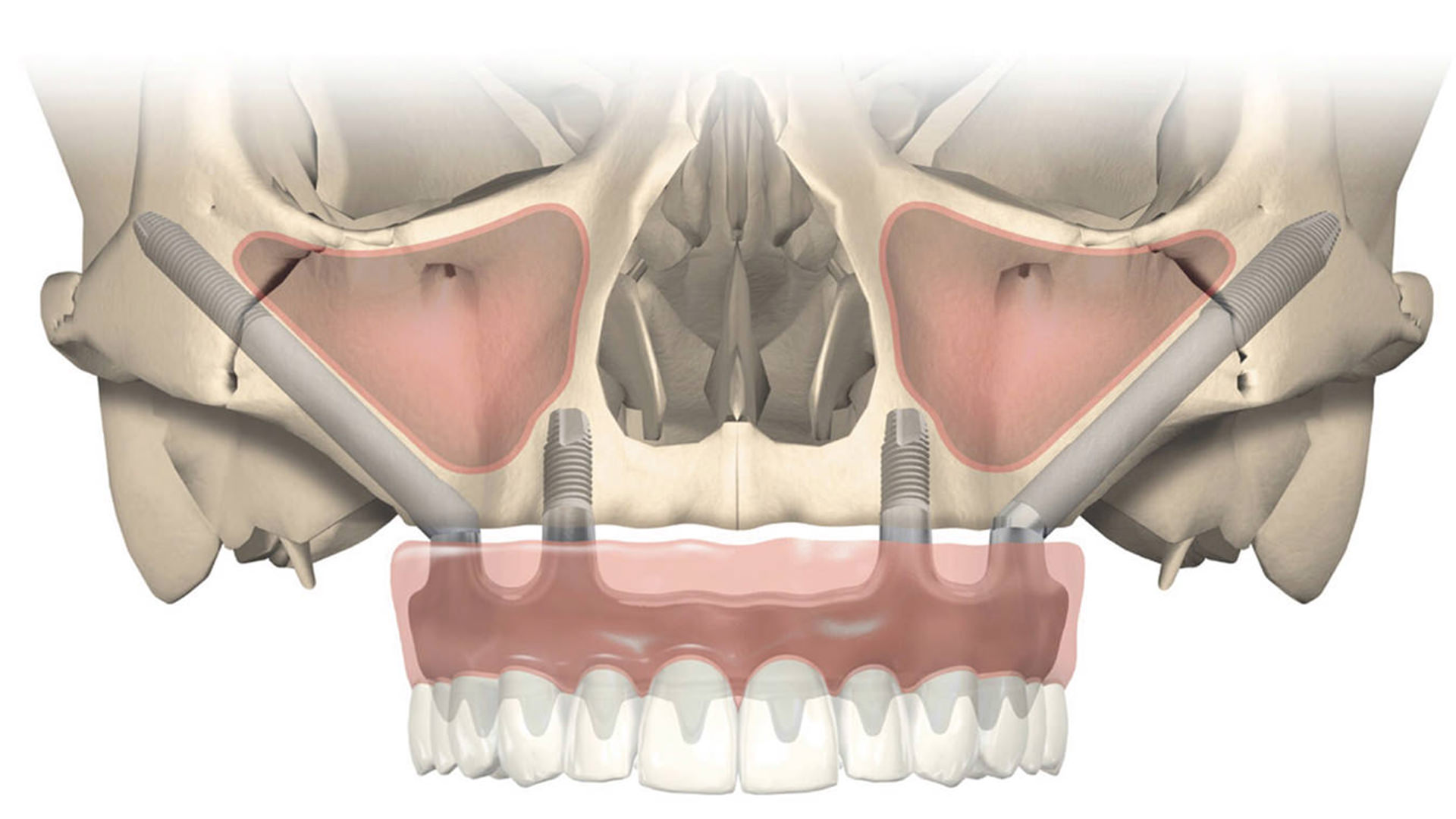
The surgical technique is called Zygomatic Implant Placement or Zygomatic Transfixation as it can be found in scientific literature.
In this context, I’m not going to go into the description of the various surgical approaches, nor the type of research that is being carried out today, both at a medical and surgical level, in order to make surgery ever safer, more predictable and with results that allow for ever better and more appropriate Oral Rehabilitation for our patients, and in scientific research.
I’m involved in various projects, whether it’s training in Portugal, where I represent the implant brand we work with, or the study and research I’m currently carrying out at the University of London, as part of my Masters in Oral and Maxillofacial Surgery. Later on, I’ll be happy to go into more detail with you and why not even share results and advances in this area, but I don’t think the purpose of this text and this blog will take you down that road.
Zygomatic implants can be used in conjunction with conventional dental implants when there is still bone remaining in the upper jaw, i.e. in cases of moderate or advanced bone resorption that we can use as fixation during surgery or in very extreme cases.
In other words, in those cases where bone resorption is severe or extreme, where the fixation of the prosthetic structure will only occur in Zygomatic Implants, where we use 2 Zygomatic Implants on each side in the most extreme cases.
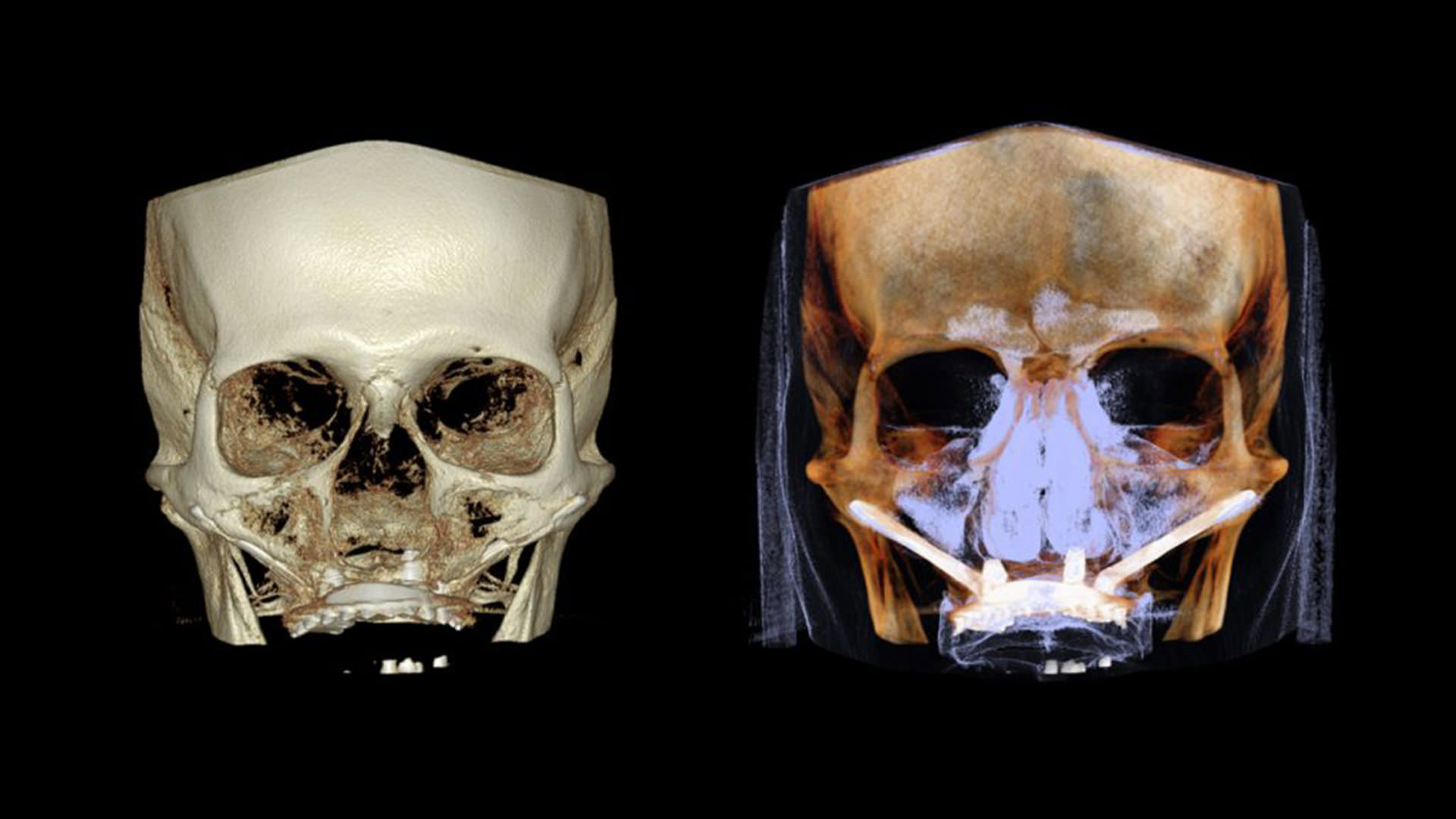
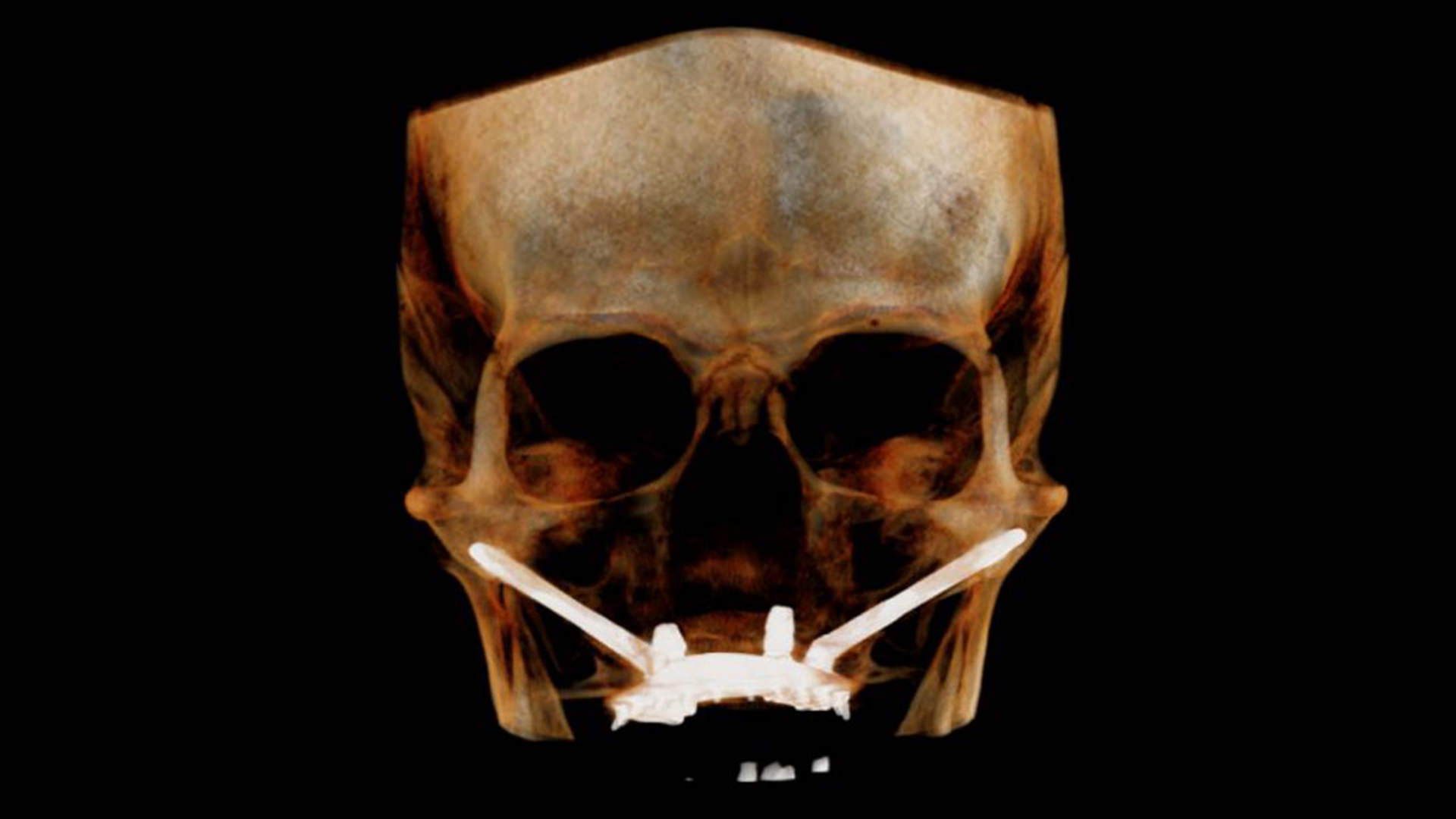
Who is a candidate for this type of treatment?
All patients in whom:
Because the degree of bone resorption is so severe or extreme, maxillary bone grafting is no longer a viable treatment option, because one of the basic principles for performing a bone graft to increase bone volume is to have enough bone remaining to fix the bone graft.
The medical and pathophysiological conditions allow this, which are measured with the set of medical, clinical, laboratory and radiology tests that we use for cases operated on under general anaesthesia. Our team operates on all patients for the placement of zygomatic implants in a hospital environment and under general anaesthesia. This therefore implies an anaesthetic consultation with our anaesthetic team.
All Patients who have or have had failed rehabilitations in the mouth, and whose planning, technique or surgical approach has not been the most appropriate, the bone remaining after removal of the failed conventional dental implants is not of sufficient volume and quality in the upper jaw to be able to repeat the surgery and return to using only conventional dental implants.
By conventional dental implants, I mean those that have a normal size and shape, within the measurements and standards accepted internationally and scientifically by all the brands authorised to market dental implants, and which are applied to the Jawbone.
Zygomatic implants are not conventional because they are larger, mainly in terms of length, and although they pass through, are supported or even fixed in the upper jaw, their main anchorage is in the zygomatic bone.
When we talk about patients with an indication for Zygomatic Implants, we are talking about a severe degree of Maxillary resorption, where any type of bone graft would prove insufficient.
A few years ago, and today to a much lesser extent, extensive surgeries were performed to harvest a large portion of bone from a donor area such as the iliac crest in order to make a graft in sufficient quantity to be able to place conventional dental implants in the upper jaw.
Over the years (studies 10 and more years after surgery) the international scientific community has recorded a high percentage of bone resorption in the grafted area, in the region of 40%, which makes the medium/long-term technique unfeasible.
And for this reason we have been developing and researching more and more in the area of zygomatic implant surgery, as evidenced by my published scientific articles and my area of scientific research being very much centred on this subject.
This is a technique used for patients with severe to extreme resorption of the upper jaw. For patients where other rehabilitation techniques with removable prostheses have failed for many years/decades. It is the latest line in solutions for the rehabilitation of atrophic jaws with fixed teeth.
The answer to this question has to be careful and a little political. Are there colleagues who don’t mind having surgery in an office environment and without general anaesthesia? Yes, there are. Others have an anaesthetist with them and do deep sedation.
In my opinion, and that of the people I’ve learned from, the Masters of Surgery, we are of the opinion that it is an invasive surgery, not just on the jaws, but on the middle third of the face, with a large operating field, with rotation instruments that are also large, and if we can do a surgery of this calibre in maximum safety in a hospital environment, under general anaesthesia, with absolute comfort and safety for the patient, why make it easier?
Dr. Luis Pinheiro and his team always perform zygomatic implants under general anaesthesia.
Zygomatic Implants Cases

Clinical Case – Zygomatic Implants | 1
Zygomatic Implants 66 years old Estoril Zygomatic implants This is a technique for patients with severe and extreme resorption of the upper jaw who wear

Clinical Case – Zygomatic Implants | 2
Zygomatic implants 49 anos Belgium Zygomatic implants This is a technique for patients with severe and extreme resorption of the upper jaw who wear full

Clinical Case – Zygomatic Implants | 4
Zygomatic Implants 59 years old Cascais Zygomatic implants This is a technique for patients with severe and extreme resorption of the upper jaw who wear

